
Introduction
Photobiomodulation therapy (PBMT) is the clinical term for what is commonly called red light therapy or low-level light therapy (LLLT). The name describes exactly what it is: using specific wavelengths of light to produce biological changes in tissue.
Understanding PBMT properly helps buyers separate credible devices from overclaimed ones - and understand what actually makes a device therapeutic versus merely emitting visible light.
Key Takeaways
- PBMT uses specific wavelengths of red or near-infrared light to produce photochemical responses in cells
- The primary mechanism involves mitochondria absorbing photons and producing cellular energy and anti-inflammatory effects
- The most studied therapeutic wavelengths are 630-670nm (red) and 810-850nm (near-infrared)
- PBMT is used for skin wellness, muscle recovery, joint support, wound healing, and other applications with varying levels of evidence
- Clinical PBMT devices operate at higher irradiance than consumer devices; the same mechanism applies at lower intensity
- Device quality - wavelength accuracy, irradiance, coverage - determines whether a consumer device delivers meaningful therapeutic effect
The Mechanism: How Light Becomes Biology
PBMT works because specific wavelengths of light are absorbed by chromophores in cells - molecular structures that respond to light of particular wavelengths.
The primary target is cytochrome c oxidase (CCO) in mitochondria. When photons at 630-670nm or 810-850nm reach CCO, they:
- Increase mitochondrial activity and ATP (cellular energy) production
- Trigger nitric oxide release, supporting local circulation
- Activate anti-inflammatory signaling pathways
- Support cellular repair and renewal processes
The practical takeaway for buyers: the mechanism is cellular, not surface. Light at the right wavelength drives a cascade of biological responses.
Which Wavelengths Are Used in PBMT
| Wavelength | Range | Primary tissue targets | Most studied for |
|---|---|---|---|
| Red | 630-700nm | Epidermis, dermis (1-4mm) | Skin wellness, wound healing, surface inflammation |
| Near-infrared | 810-1100nm | Muscle, joint, deeper tissue (4-8mm+) | Muscle recovery, joint support, neurological applications |
660nm specifically is the most researched wavelength within the red range for skin and soft tissue applications.
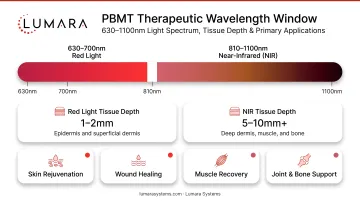
What PBMT Is Used For
Stronger evidence: wound healing, post-surgical recovery, muscle recovery, oral healing, joint pain, skin collagen improvement
Emerging evidence: hair follicle support, neurological applications, thyroid support, fertility support, and neuropathy pain support
Evidence varies significantly by condition. The fact that PBMT works for wound healing does not mean it works equivalently for every claimed application.
Clinical PBMT vs At-Home Consumer Devices
| Factor | Clinical PBMT | Consumer at-home |
|---|---|---|
| Irradiance | 50-500+ mW/cm² | 10-80 mW/cm² |
| Session length | 2-10 minutes | 5-20 minutes |
| Wavelength verification | Calibrated and certified | Varies by brand |
| Regulatory status | Medical device clearance | Ranges from none to FDA 510k |
Clinical devices deliver higher irradiance - reaching therapeutic dose faster. Consumer devices accumulate the same tissue dose over longer sessions. Wavelength accuracy becomes more critical at lower irradiance.

What Makes a Consumer PBMT Device Credible
Wavelength verification: Lumara's devices undergo triple wavelength testing to confirm 660nm output.
Irradiance at treatment distance: Ask for figures at 6" and 12" - not 0 inches.
Coverage consistency: Consistent LED density produces more even dose distribution.
FDA clearance: Lumara's Illuminate V2 is FDA cleared as a Class II medical device. Always use eye protection during sessions.

Frequently Asked Questions
What is photobiomodulation therapy?
PBMT uses specific wavelengths of red or near-infrared light to produce cellular responses. The mechanism involves light absorption by mitochondria, triggering cellular energy and anti-inflammatory effects. It is the clinical term for red light therapy.
What wavelength is used in PBMT?
The two primary therapeutic windows are 630-700nm (red) and 810-1100nm (near-infrared). 660nm and 850nm are the most commonly used individual wavelengths.
Is PBMT the same as red light therapy?
Yes. PBMT, red light therapy, and LLLT all describe the same mechanism. PBMT is the clinical term; red light therapy is the consumer term.
The Mechanism Is Real - The Device Has to Be Too
Photobiomodulation is a well-established mechanism with decades of research. The challenge in the consumer market is that the mechanism only produces results when a device actually delivers the correct wavelength at sufficient irradiance.
Lumara's Illuminate V2 - 660nm triple-verified, 1,800 LEDs, 1,200 cm², 6,000 joules in 5 minutes, FDA cleared - is built around the specifications that make PBMT work at home.


