
Introduction
Many people struggle with perioral dermatitis—a stubborn, recurring rash around the mouth and nose that resists conventional skincare and often worsens with typical acne or rosacea treatments. This inflammatory condition can be frustrating precisely because what works for acne frequently triggers POD flares. Topical steroids may offer brief relief, only to trigger severe rebound inflammation.
Light therapy offers a non-invasive path for people with inflammatory skin conditions, and this guide focuses specifically on blue light therapy for POD: what the science says, how it compares to red light, and how to use it effectively at home. Blue light has proven antibacterial and anti-inflammatory effects, but POD is not a purely bacterial condition. The answer is more nuanced than a simple yes or no.
TLDR:
- Blue light (415–420nm) destroys surface bacteria and reduces superficial inflammation, but penetrates only 1mm deep
- Red light (660nm) penetrates deeper (4–5mm), calming inflammation and supporting barrier repair—more relevant to POD's root cause
- No direct clinical trials exist for blue light on POD specifically; evidence comes from similar conditions like acne and eczema
- Combined red + blue light therapy shows superior results in inflammatory skin conditions, reducing lesions by up to 76–77%
- Light therapy works best alongside a simplified, barrier-focused routine—not as a standalone cure
What Is Perioral Dermatitis (and Why It's So Stubborn)
Perioral dermatitis is an inflammatory skin condition marked by small red bumps, papules, and sometimes pustules clustered around the mouth, nose, and occasionally the eyes. It affects roughly 0.1% to 1% of the population, primarily women between 20–45 years old.
Unlike acne, POD doesn't produce comedones (blackheads or whiteheads), and it typically spares the immediate lip border — a detail that helps clinicians distinguish it from other conditions.
POD is commonly misdiagnosed as acne or rosacea, leading patients down ineffective treatment paths. Standard acne treatments often worsen the condition because POD involves significant epidermal barrier dysfunction. Harsh exfoliants, strong actives, and continued steroid use further strip the barrier and exacerbate inflammation.
The Multifactorial Nature of POD
POD rarely has a single cause. Triggers are often layered, and identifying them is half the battle. Common contributing factors include:
- Topical corticosteroid use — Steroids suppress symptoms short-term but alter follicular microflora, triggering severe rebound flares on withdrawal and creating chronic dependency
- Fluoride-containing toothpaste — Frequently overlooked; switching to a fluoride-free formula can reduce flare frequency
- Overloaded skincare routines — Heavy occlusives like petroleum and mineral oil, plus SLS and fragrances, compromise the already-damaged skin barrier
- Hormonal fluctuations — Pregnancy and oral contraceptives can precipitate flares
- Stress — Exacerbates the inflammatory cascade
Because POD's core mechanism is barrier disruption and inflammation, many standard treatments backfire — stripping the skin further instead of calming it. That's why low-irritation alternatives like light therapy have gained traction as a gentler path forward.
How Blue Light Therapy Works Against Perioral Dermatitis
Blue light therapy uses visible light in the 400–500 nm range that penetrates the skin superficially, reaching depths of roughly 0.5–1 mm. This shallow penetration means it works primarily in the epidermis and upper dermis. Unlike UV-based therapies, blue light is UV-free and safer for regular use.
Primary Anti-Bacterial Mechanism
Blue light, particularly around 415–420 nm, activates endogenous bacterial porphyrins, triggering reactive oxygen species (ROS) production that destroys surface-level bacteria. This is the well-established mechanism behind its use in acne vulgaris and is relevant to POD given that fusobacteria and Demodex mites are implicated in its pathogenesis.
Anti-Inflammatory Pathway
Blue light modulates inflammation through two key mechanisms:
- Nitric oxide release — Blue light triggers photolytic release of nitric oxide (NO) from S-nitroalbumin in the skin
- Nrf2/NF-kB signaling — It upregulates the Nrf2 antioxidant pathway and inhibits NF-kB, reducing pro-inflammatory cytokines including IL-6, TNF-α, and IL-1α
Keratinocyte Regulation
Blue light reduces keratinocyte proliferation and regulates differentiation, which may help normalize the skin barrier disruption common in POD. Research by Sadowska et al. (2021) documented these antiproliferative effects in hyperproliferative and chronic inflammatory skin diseases.
The Limitation: Shallow Penetration
Because blue light penetrates less than 1 mm, it primarily addresses surface-level bacterial and inflammatory factors. Deeper dermal inflammation — a known driver in persistent POD flares — falls outside its reach, which is why blue light often works best as part of a broader treatment approach rather than a standalone solution.
The Evidence: Does Blue Light Actually Help Perioral Dermatitis?
Direct clinical trials on blue light therapy for perioral dermatitis (POD) are extremely limited. Most of what we know comes from adjacent inflammatory conditions — which is worth stating upfront rather than burying.
Evidence From Analogous Conditions
Research on related inflammatory skin conditions shows consistent, measurable results:
- Acne vulgaris — An RCT using 414 nm blue light (17.6 J/cm²) every other day for 8 weeks showed a 50.08% decrease in lesion counts
- Atopic dermatitis — A trial using 453 nm blue light 3 times per week for 4 weeks showed statistically significant improvement in the local Eczema Severity Index
- Itch reduction — Full-body 450 nm blue light significantly reduced itch scores in atopic dermatitis patients
These results are relevant to POD given its overlap of inflammatory and bacterial components.
Real-World and Dermatologist Validation
While POD-specific clinical trials are lacking, real-world accounts and dermatologist commentary offer useful context — though it's worth noting these examples reference red light therapy, not blue. Both wavelengths address inflammatory pathways, making the overlap relevant even if the mechanisms differ.
- A beauty journalist reported clearing a POD flare-up using a red/yellow LED mask for 10 minutes nightly
- Dr. Dara Spearman states: "Red light therapy is great for reducing inflammation and redness. It can also speed up healing and calm the skin"
- Dr. Anjali Mahto commented: "Red light can be anti-inflammatory, so it may well be helping... I wouldn't tell someone who felt it was benefitting them to stop"
When Blue Light Is Most Likely Helpful
Blue light tends to be most useful for POD in early or mild flare-ups, where surface-level inflammation and possible microbial activity are driving the reaction. Severe or persistent cases often need more than light therapy can offer on its own — prescription treatments, trigger identification, and barrier recovery all play a role.
That said, blue light isn't meant to be a standalone solution. It works best alongside a stripped-back skincare routine that removes known irritants and lets the skin recover, with light therapy functioning as a support tool rather than the primary intervention.
Blue Light vs. Red Light for Perioral Dermatitis: Which Should You Choose?
Comparing Primary Mechanisms
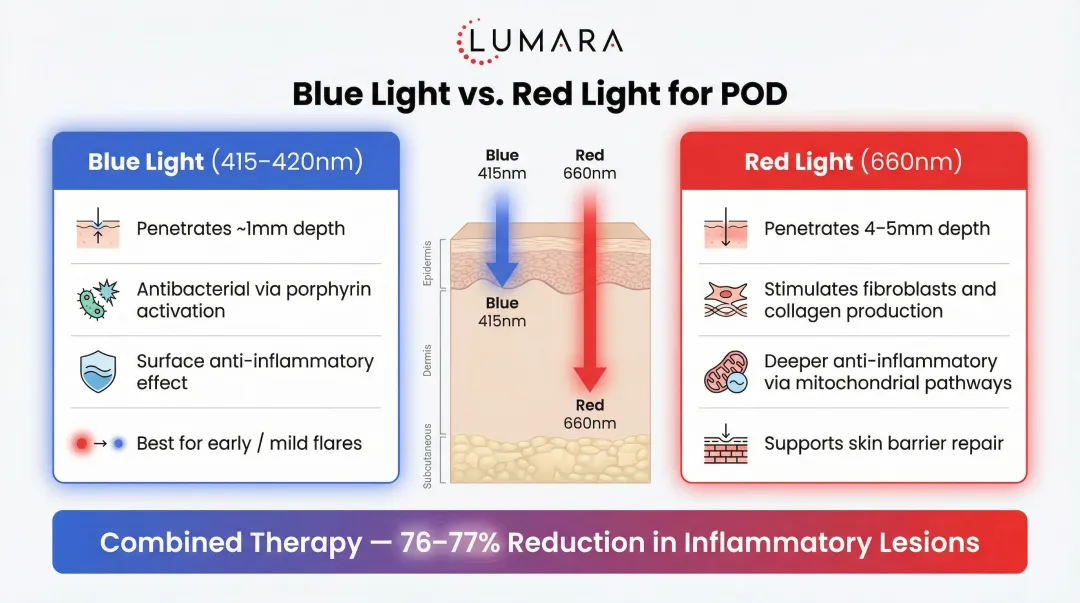
Blue light (400–470 nm):
- Penetrates ~1 mm into the epidermis
- Antibacterial via porphyrin activation
- Surface anti-inflammatory action
Red light (630–700 nm):
- Penetrates 4–5 mm into the dermis
- Stimulates fibroblast growth factors and collagen production
- Stronger documented anti-inflammatory effects via mitochondrial photobiomodulation
Red light's deeper penetration allows it to stimulate fibroblast proliferation, enhance collagen synthesis, and reduce pro-inflammatory cytokines, aiding in barrier repair and wound healing.
Red Light: The Stronger Anti-Inflammatory Option
POD is primarily an inflammatory barrier condition — not a bacterial infection. That distinction matters when choosing a light modality. Red light targets the deeper pathways driving POD:
- Modulates inflammatory cytokines in the dermis
- Supports skin barrier recovery through fibroblast stimulation
- Reduces visible redness at the surface
As Dr. Spearman notes, "Red light therapy is great for reducing inflammation and redness. It can also speed up healing and calm the skin."
The Case for Combined Therapy
Research on acne shows combined red + blue light produces superior outcomes compared to either alone. One RCT using mixed blue (415 nm) and red (660 nm) light daily for 15 minutes achieved a 76% mean improvement in inflammatory lesions. Another study using 420 nm blue and 660 nm red light for 2.5 minutes twice daily resulted in a 77% decrease in inflammatory lesions.
POD shares this multifactorial profile — surface bacterial imbalance combined with deeper inflammatory disruption. Combined therapy addresses both layers at once, which may explain why the data on mixed-wavelength protocols is consistently stronger than single-wavelength approaches.
Home-Use Red Light Devices
For home use, a dedicated facial red light device delivers more consistent exposure than handheld wands or repurposed panels. Lumara Systems' VISO Red Light Therapy Mask is built around the 660nm wavelength shown in the combined-therapy research above, with 470 embedded LEDs across the full facial surface and a splash-safe build suited for daily skincare routines. Treatment sessions run five minutes — low enough friction to stay consistent over a multi-week protocol.



