What the Research Shows
Introduction
Post-oral surgery pain and swelling are driven by an inflammatory response that standard care manages primarily with NSAIDs, corticosteroids, and in some cases opioids. Red light therapy has emerged as a non-pharmaceutical adjunct with a growing evidence base - particularly for wisdom tooth extractions and implant placements.
This guide covers what the clinical research shows, which procedures have the strongest evidence, how to use red light therapy after oral surgery, and what to look for in a device that fits a home recovery routine.
Key Takeaways
- Red light therapy at 660nm has documented evidence as a post-oral surgery adjunct for pain, swelling, and trismus (restricted mouth opening)
- A 2023 JADA scoping review of 22 RCTs found meaningful benefits with zero adverse events reported
- The most robust evidence is for mandibular third molar (wisdom tooth) extractions
- Same-day application after surgery is considered safe in the clinical literature
- Near-infrared wavelengths (around 808nm) are used in some protocols for deeper tissue and bone-level recovery
- Device quality - wavelength accuracy and output consistency - determines whether home use can replicate clinical results
Why Post-Oral Surgery Recovery Is Difficult to Manage
Oral surgery triggers an acute inflammatory response: prostaglandin release drives pain, cytokine signaling drives swelling, and tissue disruption at the surgical site requires structured healing. Standard pharmaceutical approaches work, but they carry tradeoffs - NSAIDs have GI implications with extended use, and stronger analgesics carry dependency risk.
Red light therapy does not replace pharmaceutical pain management for acute post-surgical pain. It is used alongside it to support the body's healing response, reduce inflammatory load, and shorten the recovery window.
How Red Light Therapy Works After Oral Surgery
Red light at 660nm is absorbed by tissue at depths of 1-4mm, which covers the gingival tissue and superficial structures most affected by oral surgery. Near-infrared light at wavelengths around 808nm penetrates deeper - reaching bone and periosteal tissue, which is more relevant for implant procedures and socket healing. For a deeper comparison of red versus near-infrared wavelengths, see the difference between infrared and red light therapy.
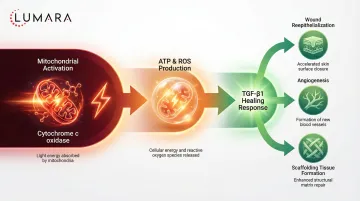
The proposed mechanisms include:
- Reduced pro-inflammatory signaling, particularly TRPV1 modulation which is associated with pain perception
- Support for lymphatic drainage, which reduces post-surgical edema
- Cellular energy support at the wound site, which may accelerate tissue repair
- Improved microcirculation to healing tissue
These mechanisms align with the outcomes measured in clinical trials: reduced pain scores, reduced swelling, and faster return of normal mouth opening.
JADA 2023 Scoping Review
A scoping review published in the Journal of the American Dental Association examined 22 randomized controlled trials of photobiomodulation after oral surgery. For a broader look at recent photobiomodulation research, see the 2025 red light therapy clinical trial roundup. The review found consistent benefits for pain reduction, swelling reduction, and trismus improvement across the included trials. Zero adverse events were reported across all 22 studies.
This is a meaningful safety signal: red light therapy's post-surgical adverse event profile in controlled trials is consistently clean.
2024 Meta-Analysis: Wisdom Tooth Extractions
A 2024 meta-analysis focused specifically on mandibular third molar extractions - the most common major oral surgery procedure - and pooled data from 22 studies covering 989 subjects. It found statistically significant reductions in post-operative pain and swelling in the photobiomodulation groups compared to controls.
Mandibular third molars are particularly relevant because of their proximity to nerve structures and the complex nature of their surgical removal, making post-operative pain management a meaningful clinical challenge.
Implant Surgery Evidence
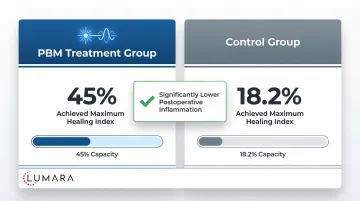
A 2023 RCT examining photobiomodulation after dental implant placement found 45% of treated patients achieved complete healing within the monitored period, compared to 18.2% in the control group. The trial used a combination of 630nm and 808nm wavelengths - targeting both superficial tissue and deeper bone-level healing.
How to Use Red Light Therapy After Oral Surgery
Timing
Same-day application after surgery is supported in the clinical literature and is used in clinical trials. The goal is to intervene at the beginning of the inflammatory response rather than after it is established.
A typical home protocol follows this structure:
- Day 0 (same day): First session as soon as comfortable after returning home
- Days 1, 3, 5, 7: Follow-up sessions through the first week
- Week 2 onward: Sessions every 2-3 days as healing continues
Positioning and Session Length
For home use with a panel device, the treatment area is the cheek and jaw overlying the surgical site. Maintain a consistent distance from the device per manufacturer guidance - typically 6-12 inches for panels.
Session length depends on device irradiance. For a 660nm panel at 30 mW/cm², 5-10 minutes per side is within the parameters used in clinical protocols.
What to Avoid
- Do not apply light directly to an open wound without clinical guidance
- Do not use if you have received radiation therapy to the head or neck recently
- If sutures are in place, consult your oral surgeon before starting home photobiomodulation
- Do not use as a substitute for prescribed pharmaceutical pain management in the acute post-surgical period
At-Home Device Selection
The clinical trials that established post-oral surgery evidence used calibrated devices with precise wavelength output. Replicating those results at home requires a device that delivers consistent 660nm output with verified accuracy.
Lumara's Illuminate V2 is a 660nm red light panel built around verified wavelength precision, with 1,800 LEDs across a 1,200 cm² treatment area, a 5-minute session format, and a splash-safe build suited to daily use. At 6,000 joules per session and FDA cleared, it provides the output parameters that make at-home protocols comparable to clinical trial protocols.
Frequently Asked Questions
Can I use red light therapy after oral surgery?
Yes. Clinical trials have documented red light therapy as a safe adjunct for post-oral surgery recovery. A 2023 JADA scoping review of 22 RCTs reported zero adverse events. Start with same-day application if comfortable, and continue sessions through the first week of recovery.
How soon after oral surgery can I start red light therapy?
Clinical protocols support same-day application. The goal is to begin early in the inflammatory response. Most home users begin within a few hours of returning home after their procedure.
Does red light therapy help with dental implant healing?
Yes. A 2023 RCT found significantly higher complete healing rates in the photobiomodulation group versus controls at the measured endpoint. Implant protocols often include near-infrared wavelengths (around 808nm) in addition to 660nm to address deeper bone-level tissue.
How many sessions do I need after oral surgery?
Clinical protocols typically use sessions on days 0, 1, 3, 5, and 7, then every 2-3 days in week two. Individual recovery varies; the first week of consistent sessions is the most important period.
Is red light therapy safe to use after gum surgery?
Yes. Gum surgery is one of the oral surgery categories included in photobiomodulation trials, with consistent findings on reduced swelling and improved tissue healing. Use as you would for other post-oral surgical procedures.
What wavelength should I use for oral surgery recovery?
660nm is the most studied wavelength for soft tissue recovery. Near-infrared around 808nm is used in some protocols for deeper tissue and bone. For home use, 660nm panels address the most common soft-tissue post-surgical recovery needs.
Recovery Is Where Device Quality Pays Off
The clinical evidence for red light therapy after oral surgery is some of the strongest in any consumer light therapy application - 22 RCTs in a single JADA review, with zero adverse events and consistent outcome benefits.
Whether those results can be replicated at home depends on having a device that actually delivers the right wavelength at the right output. Lumara's Illuminate V2 - 660nm, 1,800 LEDs, 6,000 joules per 5-minute session, FDA cleared, Made in the USA - is built around that standard.