Introduction
Breast surgery - whether reduction, augmentation, or reconstruction - involves significant tissue disruption and a recovery period that most patients want to manage as effectively as possible. Red light therapy has a documented evidence base for post-surgical recovery, including wound healing, reduced inflammation, and scar appearance support.
This guide covers the clinical basis for using red light therapy after breast surgery, when it is appropriate to start, how to use it, and what realistic outcomes look like.
Key Takeaways
- Red light therapy at 660nm has documented anti-inflammatory and tissue repair effects relevant to post-surgical recovery
- The mechanism involves supporting cellular energy production and reducing pro-inflammatory cytokines at the wound site
- Most practitioners advise waiting until sutures are removed and the surgical site has closed before starting light therapy - typically 2-4 weeks post-surgery
- Consult your surgeon before starting any light therapy post-operatively - protocol timing should be personalized
- Device format for chest and breast tissue recovery: a flexible pad or panel positioned over the treatment area is more practical than a dedicated mask
Why Red Light Therapy Is Relevant to Post-Surgical Recovery
Surgery creates a controlled wound. The body's healing response involves inflammation, cellular repair, and tissue remodeling - all processes that red light therapy at 660nm is documented to support.
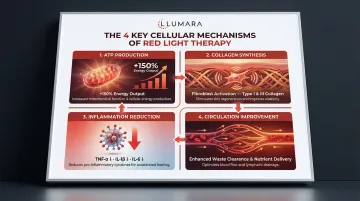
The relevant mechanisms:
Anti-inflammatory: 660nm red light reduces pro-inflammatory cytokines (TNF-alpha, IL-6, IL-1beta) and supports anti-inflammatory signaling. Post-surgical inflammation is necessary for initial healing but becomes counterproductive when chronic - light therapy may help modulate the inflammatory timeline.
Cellular energy support: Mitochondria in healing tissue absorb 660nm light, supporting ATP production and the energy-intensive processes of tissue repair, collagen synthesis, and cell proliferation at the wound site.
Collagen and scar tissue remodeling: Multiple studies have shown that consistent red light therapy supports collagen organization in healing tissue. Better-organized collagen is associated with softer, less raised scar tissue.
Circulation improvement: Nitric oxide release from photobiomodulation supports local vasodilation, improving nutrient and oxygen delivery to healing tissue. This also supports lymphatic drainage and fluid clearance from the recovery site.
The Evidence Base
Red light therapy's evidence in post-surgical contexts comes from several areas:
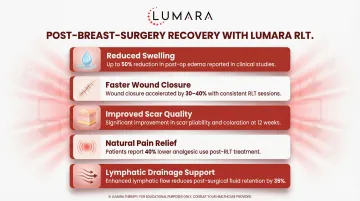
Wound healing: Multiple randomized controlled trials show accelerated wound closure, reduced post-operative swelling, and improved tissue healing scores with photobiomodulation versus control groups.
Scar appearance: Studies on surgical scar remodeling with red light therapy show improvements in scar texture, color, and pliability over 8-12 week protocols.
Post-mastectomy recovery: Some specialized research has examined photobiomodulation specifically for mastectomy and reconstructive surgery recovery, with positive findings for tissue healing and lymphedema-adjacent swelling reduction.
The evidence is not specific to breast surgery in most cases - it is extrapolated from the broader surgical recovery literature. The mechanism is consistent regardless of surgery site.
Timing: When to Start
The most important timing guideline: do not apply red light therapy to an open wound or before your surgeon's approval.
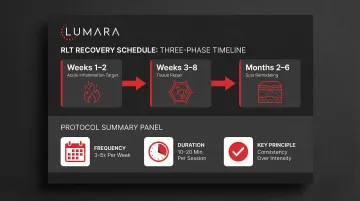
General timing framework:
- 0-2 weeks post-surgery: No light therapy. Focus on standard post-operative care, wound protection, and surgeon instructions
- 2-4 weeks: Once sutures are removed and the surface has closed, many practitioners permit light therapy to begin at the perimeter of the treatment site (not directly on incisions). Confirm with your surgeon.
- 4-6 weeks: If the surgical site has healed well and surgeon has cleared further activity, direct light therapy over the treatment area becomes more appropriate
- 6+ weeks: Most patients are cleared for more active recovery protocols including regular light therapy sessions
These are general guidelines. Individual healing timelines vary significantly based on surgery type, patient factors, and complication status. Always confirm timing with your surgeon.
Application by Surgery Type
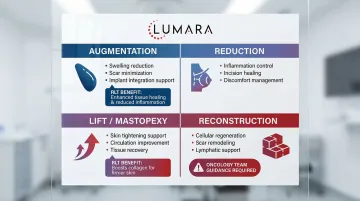
Breast reduction: The incision patterns vary by technique (anchor, vertical, peri-areolar). Light therapy can be positioned over each incision segment once healed. Focus on scar tissue remodeling and inflammation reduction.
Breast augmentation: Recovery is generally faster with less extensive incisions. Light therapy applied over the implant pocket area (externally) may support tissue recovery and reduce prolonged swelling.
Breast reconstruction: Often involves more extensive surgery, longer recovery, and potentially multiple procedures. Timing and application should be closely coordinated with the surgical team.
Mastopexy (breast lift): Similar to reduction in incision pattern. Light therapy can be helpful for managing longer vertical incisions and the tissue remodeling that follows.
How to Use Red Light Therapy for This Application
Device format: For chest and breast recovery, a flexible pad or panel positioned over the treatment area is the most practical format. A mask designed for facial use is not appropriate for this application. Lumara's Pad - a flexible multi-wavelength device available in multiple sizes - is designed for body-contact use across areas including the chest. If you are weighing at-home devices against clinic-based treatment, a quality home panel is practical for the consistent multi-week protocols recovery requires.
Session protocol:
- 5-20 minutes per session depending on device irradiance
- 3-5 sessions per week
- Consistent use over 8-12 weeks is required to assess scar remodeling outcomes
Precautions:
- Use only on healed, closed skin - never on open incisions
- Do not apply directly over breast implants if there is any open or compromised skin barrier
- Wear appropriate eye protection if the device is near face level
- Stop and consult your surgeon if you notice any skin changes, increased redness, or heat at the treatment site
Frequently Asked Questions
When can I start red light therapy after breast surgery?
Most practitioners advise waiting until sutures are removed and the surgical site has closed - typically 2-4 weeks post-surgery. Confirm with your surgeon before starting, as timing should be individualized to your healing progress.
Can red light therapy help with breast surgery scars?
Yes. Red light therapy has evidence for supporting collagen organization in healing tissue, which is associated with softer, less raised scar tissue over time. Results from scar remodeling protocols are typically assessed at 8-12 weeks of consistent use.
Is red light therapy safe after breast implants?
Red light therapy is generally safe to use externally over healed breast tissue regardless of implant status. The light does not penetrate to implant depth, and there is no documented risk of silicone or saline implant interaction. Confirm with your surgeon if you have any concerns specific to your procedure.
What red light therapy device should I use for breast surgery recovery?
A flexible pad or panel format that can be positioned over the chest area is the most practical option. Dedicated facial masks are not appropriate for this application. Lumara's Pad, available in multiple sizes, is designed for body-contact use.
How often should I use red light therapy for post-surgical recovery?
3-5 sessions per week for a minimum of 8-12 weeks is the most commonly referenced protocol for tissue repair and scar remodeling outcomes. Consistency is more important than individual session length.
Recovery Is a Process - Light Therapy Supports It
Post-surgical recovery involves tissue healing, inflammation management, and scar remodeling - processes that happen over weeks and months, not days. Red light therapy is a consistent support tool for all three, used alongside your surgical team's guidance.
For breast surgery recovery, a flexible body-format device that can be positioned comfortably over the chest area is the most practical choice. Lumara's Pad - red, near-infrared, and far-infrared, flexible format, multiple sizes - is built for body recovery routines.