
Introduction
Period pain - clinically termed dysmenorrhea - affects a significant portion of people who menstruate, ranging from mild discomfort to pain severe enough to disrupt daily activity. Pharmaceutical approaches (NSAIDs, hormonal contraceptives) are the standard, but interest in non-pharmaceutical adjuncts has grown.
Red light therapy at 660nm has been used in pain management research for various musculoskeletal and inflammatory conditions. Its application to menstrual pain is a newer but plausible extension of that work. This guide covers what is known, what is proposed, how to use it, and what realistic expectations look like.
Key Takeaways
- Red light therapy at 660nm has documented evidence for reducing pain in inflammatory and musculoskeletal conditions; its application to period pain follows the same mechanism
- Dysmenorrhea involves uterine muscle contractions and prostaglandin-driven inflammation - mechanisms that red light therapy has a plausible pathway to address
- Direct RCT evidence specific to menstrual pain is limited; the evidence base is extrapolated from analogous pain conditions
- Red light therapy is used as an adjunct alongside, not a replacement for, standard pain management approaches
- Device quality matters: wavelength accuracy and coverage are the key specs for consistent results
What Causes Period Pain
Dysmenorrhea is primarily caused by prostaglandin-driven uterine contractions. During menstruation, prostaglandins trigger smooth muscle contractions in the uterus to facilitate the shedding of the endometrial lining. Elevated prostaglandin levels correlate with stronger contractions and more severe pain.
Secondary dysmenorrhea - pain associated with conditions like endometriosis or fibroids - has additional contributing factors beyond prostaglandins. Red light therapy research does not distinguish clearly between primary and secondary dysmenorrhea in the limited literature available.
How Red Light Therapy Applies to Period Pain
The mechanism pathway from red light therapy to period pain relief is not unique to menstrual conditions. It follows the same anti-inflammatory and circulation-support pathway documented in musculoskeletal and wound healing research.
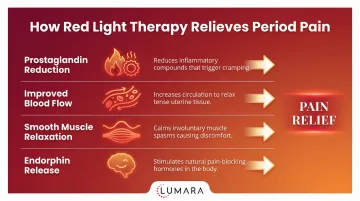
At 660nm, red light is absorbed by tissue and supports:
- Reduced pro-inflammatory cytokine activity, which may lower prostaglandin-driven inflammation
- Improved local circulation, which helps clear inflammatory mediators from tissue
- Muscle relaxation responses, relevant to smooth muscle cramping
The tissue penetration at 660nm is approximately 1-4mm, reaching superficial abdominal and pelvic tissue. For deeper uterine tissue, near-infrared wavelengths at 808-850nm would be more relevant anatomically, though the consumer evidence for these specific applications is limited.
What the Research Shows
Direct RCT evidence for red light therapy specifically targeting dysmenorrhea is limited. Most of the relevant literature comes from:
- Musculoskeletal pain studies: Multiple trials on low back pain and pelvic floor conditions have shown meaningful pain reductions with photobiomodulation, including a 2022 systematic review showing significant pain reduction in chronic musculoskeletal conditions
- Gynecological inflammation research: Some small trials have examined photobiomodulation for endometriosis-related pain, with preliminary positive findings but limited sample sizes
- Menstrual pain specific trials: A small number of studies have examined low-level laser therapy for dysmenorrhea directly; findings have been positive but these studies are not yet sufficient for strong clinical recommendations
The honest framing: the mechanism is plausible, early evidence is encouraging, but this is not the most robustly evidenced application of red light therapy. It is used as a supportive approach alongside standard care, not as a standalone treatment.
How to Use Red Light Therapy for Period Pain
Device Placement
For period pain, the device is positioned over the lower abdomen - the area from the navel to the pubic bone. Consistent positioning over the treatment area is important for reproducible results.
Session Timing
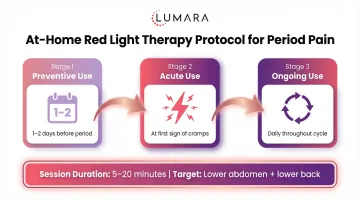
Most users find red light therapy most useful when used at the onset of pain or as a preventive approach in the days before menstruation begins. Sessions during active cramping can be used for immediate relief support; consistent sessions in the days before and during the first 1-2 days of menstruation may reduce overall inflammatory load.
A practical protocol:
- 5-10 minutes over the lower abdomen, daily or twice daily during the menstrual phase
- Begin 2-3 days before expected onset if using preventively
What to Use
A 660nm panel format positions well over the lower abdomen and provides even coverage across the treatment area. Lumara's Illuminate V2 delivers 6,000 joules of 660nm light in a 5-minute session across 1,200 cm², making it practical for daily abdominal use without extended session times.
For users who prefer a flexible pad format that conforms to body contours, Lumara's Pad - available in multiple sizes and using red, near-infrared, and far-infrared wavelengths - is designed for body-contact use and may be more comfortable for lower abdominal placement during cramps.
What Realistic Expectations Look Like
Red light therapy for period pain is not a pharmaceutical-grade intervention. Users who have tried it report variable results - some find meaningful relief, others notice minimal effect. The variability is consistent with what would be expected from an adjunct approach where individual inflammatory profiles, device quality, and protocol consistency all contribute to outcomes.
It is most appropriate to position it as a tool that may reduce the intensity and duration of cramps for some users, used alongside rather than instead of effective pain management. If period pain is severe, disruptive, or worsening, a medical evaluation to rule out secondary causes is more important than a device purchase.
Device Selection: What Matters
For period pain, the relevant device criteria are the same as for any body-focused red light application:
- Wavelength accuracy: 660nm is the most studied wavelength for soft tissue anti-inflammatory and pain applications
- Coverage area: A larger panel or pad covers the lower abdominal area more evenly than a small handheld device
- Output: Sufficient joules per session to deliver a meaningful tissue dose
- Format comfort: A pad or panel that can be positioned comfortably while lying down makes session consistency easier
Lumara's Illuminate V2 (660nm panel, 1,800 LEDs, 1,200 cm², 5 minutes, FDA cleared) and Lumara Pad (red/NIR/FIR flexible pad, multiple sizes, 20-30 minute sessions) both fit body-focused use cases where comfortable positioning during a session matters.

Frequently Asked Questions
Does red light therapy help with period pain?
Red light therapy at 660nm has plausible anti-inflammatory and circulation mechanisms relevant to menstrual pain. Direct RCT evidence specific to dysmenorrhea is limited, but extrapolated evidence from musculoskeletal and pelvic pain conditions is encouraging. It is used as a supportive adjunct alongside standard pain management, not as a replacement.
Where do you put red light therapy for period pain?
Over the lower abdomen - from the navel to the pubic bone. Consistent positioning is important for reproducible results. Sessions of 5-10 minutes at 660nm are a practical starting point.
How long does it take for red light therapy to help with cramps?
Some users report relief during or shortly after a session; others notice reduced pain intensity over several days of consistent use. Using it preventively in the days before menstruation begins, in addition to during the active pain phase, gives more opportunity for cumulative anti-inflammatory effect.
Can I use red light therapy for endometriosis pain?
Preliminary research on photobiomodulation for endometriosis-related pain exists, with some positive findings. The evidence is not yet strong enough for clinical recommendations, but the mechanism is plausible. Use it as a supportive approach alongside medical management of the condition.
Is red light therapy safe to use on the lower abdomen?
Yes. Red light therapy at 660nm applied to external abdominal tissue is considered safe. Avoid use over areas of active skin damage or rash. Standard safety precautions (eye protection if the device is near face level) apply.
What wavelength is best for period pain?
660nm is the most studied for soft tissue pain and inflammation. Near-infrared at 808-850nm penetrates deeper and may be relevant for reaching pelvic tissue, though consumer evidence for this specific application is limited. Lumara's Pad includes red, NIR, and FIR wavelengths for broader body-level coverage.
A Practical Adjunct for Monthly Pain Management
Period pain is one area where adding a non-pharmaceutical tool to the routine makes practical sense - particularly for users who find NSAIDs insufficient or prefer to reduce pharmaceutical use where possible.
Red light therapy at 660nm is not a cure for dysmenorrhea, but its mechanism aligns with the inflammatory drivers of period pain, and early evidence supports its use as a supportive approach. The right device for this use case is one with accurate wavelength delivery, sufficient coverage, and a format that is comfortable for lower abdominal sessions.
Lumara's Illuminate V2 - 660nm, 1,800 LEDs, 1,200 cm², 5-minute sessions, FDA cleared, Made in the USA - is built for consistent, accurate 660nm delivery in a panel format suited to body use.


