Introduction
ACL reconstruction involves significant tissue disruption - the graft site, surrounding soft tissue, and the broader joint environment all require sustained recovery over months. Red light therapy (photobiomodulation) is used as a non-pharmaceutical adjunct during this recovery period, and there is a meaningful evidence base for its application to post-surgical tissue healing, inflammation management, and muscle recovery.
This guide covers what the evidence shows, when to start, how to incorporate it alongside physical therapy, and which device format makes practical sense for the knee.
Key Takeaways
- Red and near-infrared light therapy has evidence for reducing post-surgical inflammation, supporting tissue repair, and accelerating muscle recovery
- Near-infrared (810-850nm) penetrates deeper than red light and is more relevant for joint and deeper tissue applications
- Most surgeons and physical therapists recommend starting light therapy after sutures are removed and the incision has closed - typically 2-4 weeks post-surgery
- Consistent sessions 3-5x per week are more important than any individual session
- Device format matters: a flexible pad that wraps around the knee is more practical than a flat panel for joint recovery
- Red light therapy works alongside PT, not instead of it
The Evidence for ACL Recovery
Inflammation and Swelling Management
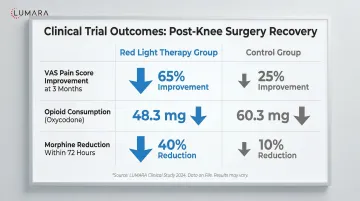
Post-surgical inflammation is necessary for healing but becomes counterproductive when chronic. Photobiomodulation reduces pro-inflammatory cytokines (TNF-a, IL-6) and supports anti-inflammatory signaling. Multiple controlled studies show reduced post-operative swelling and faster return to baseline in treated versus control groups.
Muscle Recovery and Strength
Quadriceps atrophy is one of the primary challenges in ACL recovery. Near-infrared therapy applied to the anterior thigh has evidence for reducing muscle atrophy and supporting faster strength recovery in the post-surgical period. Research on photobiomodulation for muscle recovery consistently shows reduced DOMS and improved recovery metrics.
Tissue Repair Support
Red and near-infrared light supports cellular energy and collagen synthesis in healing tissue. For the graft site, this means supporting the ligamentization process - the conversion of the graft into functional ligament tissue.
When to Start After ACL Surgery
Do not apply light therapy to the knee before your surgeon clears it. Standard timing guidelines:
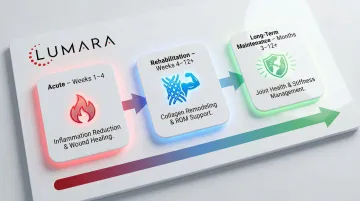
0-2 weeks post-surgery: Focus on standard post-operative care (ice, compression, elevation, prescribed PT exercises). Light therapy directly over the incision is not recommended during this period.
2-4 weeks: Once the incision has closed and sutures are removed, most physical therapists and surgeons are comfortable with light therapy beginning at the periarticular area (around but not directly over the incision).
4+ weeks: Direct application over the joint area becomes more appropriate as healing progresses. Sessions can be more targeted and more frequent.
Always confirm timing with your surgeon or physical therapist - individual healing timelines vary.
How to Use It Alongside Physical Therapy
Red light therapy is most effective when used as part of a comprehensive recovery approach:
Pre-PT session: Apply light therapy 15-30 minutes before physical therapy to support circulation and reduce pre-existing inflammation in the joint. Many users find this helps with joint mobility during the session.
Post-PT session: Apply light therapy after PT to support recovery from the exercise stress and reduce post-session soreness.
Independent sessions: On non-PT days, light therapy sessions maintain anti-inflammatory support and support the overall healing environment.
Session protocol:
- 20-30 minutes per session (pad format)
- 3-5 sessions per week
- Cover the knee, surrounding tissue, and the anterior thigh (for quadriceps support)
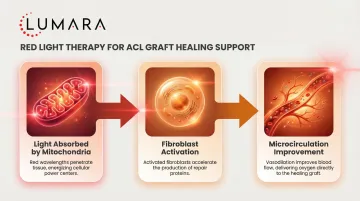
Why Device Format Matters for ACL Recovery
The knee is a complex three-dimensional structure. A flat panel positioned at a distance from the joint does not maintain consistent proximity to all joint surfaces simultaneously. A flexible pad that conforms around the knee provides:
- More consistent LED-to-tissue contact across the joint surface
- Coverage of the popliteal area (back of knee) in addition to the anterior face
- Comfortable positioning during extended sessions without manual maintenance
Lumara's Pad - available in multiple sizes (the 11x11" and 8x17" sizes work well for knee coverage), with red, near-infrared, and far-infrared wavelengths - is designed for exactly this type of body-contact joint application. The near-infrared component provides the depth penetration relevant for joint tissue; the red and far-infrared components support surface tissue and circulation.
Frequently Asked Questions
Can red light therapy help ACL recovery?
Yes, as a complement to physical therapy and medical care. Evidence supports photobiomodulation for reducing post-surgical inflammation, supporting muscle recovery, and accelerating tissue repair. Results depend on consistent use and correct timing relative to the surgical healing phases.
When should I start red light therapy after ACL surgery?
Most practitioners recommend starting after sutures are removed and the incision has closed - typically 2-4 weeks post-surgery. Always confirm with your surgeon before starting.
How often should I use red light therapy for ACL recovery?
3-5 sessions per week, 20-30 minutes per session using a pad format over the knee and surrounding tissue. Consistency over weeks is more important than any individual session.
What wavelength is best for ACL recovery?
Near-infrared (810-850nm) is the most relevant for deep joint tissue. Red light (660nm) contributes anti-inflammatory effects at the surface. Devices combining both wavelengths cover more of the relevant tissue depth.
Is light therapy safe after knee surgery?
Generally yes, after the incision has closed and with surgeon approval. Avoid direct application over open incisions or actively healing wounds. Use a timer rather than sensation-based feedback for post-surgical tissue with reduced sensitivity.
Support Your Recovery With Consistent, Targeted Treatment
ACL recovery is a months-long process. Red light therapy is a consistent supportive tool - not a shortcut, but a meaningful addition to a comprehensive rehabilitation program.
For knee and joint recovery, Lumara's Pad - flexible format, red/NIR/FIR wavelengths, multiple sizes, 3-year warranty - provides the direct-contact coverage that makes knee sessions practical and consistent.