
Introduction
Near-infrared light therapy for depression and mental health is one of the more actively researched frontier applications of photobiomodulation. It is not an established treatment in psychiatry, and it is not FDA cleared for depression. But the mechanistic basis is coherent, early clinical studies are encouraging, and the research is advancing faster than in many niche photobiomodulation applications.
This guide covers what the science shows, what clinical studies have found, realistic expectations, and how to think about NIR therapy in the context of mental health support.
Key Takeaways
- Near-infrared light (810-850nm) penetrates into brain tissue through the skull and scalp at consumer device irradiance levels
- The proposed mechanism involves mitochondrial support in neurons - relevant because neuronal energy deficits are associated with depression
- Multiple small clinical trials have shown improvements in depression symptoms with transcranial NIR therapy
- Evidence is promising but not yet definitive - large-scale RCTs are still limited
- NIR therapy is not a replacement for psychiatric care, medication, or established therapies; it is most appropriate as a complementary approach
- Consult a mental health professional before making any changes to depression treatment
Why the Mechanism Is Plausible
Neurons are among the most metabolically demanding cells in the body. They require enormous amounts of ATP (cellular energy) to maintain electrochemical gradients, neurotransmitter synthesis, and signal transmission. Mitochondrial dysfunction in neurons is increasingly associated with depression and other mood disorders.
Near-infrared at 810-850nm is absorbed by cytochrome c oxidase in mitochondria - the same cellular target as red light therapy, but at greater depth. The relevant insight for brain applications is penetration: NIR wavelengths can pass through the skull and scalp to reach cortical tissue.
At consumer device irradiance levels, meaningful amounts of NIR light reach superficial brain tissue - enough to potentially stimulate mitochondrial activity in neurons. This is the mechanistic basis for research interest in transcranial photobiomodulation (tPBM) for neurological and psychiatric conditions.
What the Research Shows
Emerging Clinical Evidence
A growing body of small clinical trials and case series has examined transcranial NIR therapy for depression and other neuropsychiatric conditions:
- Several pilot studies using 810nm and 850nm NIR applied to the forehead have shown improvements in Hamilton Depression Rating Scale scores and self-reported mood measures in treated versus control groups
- Some studies have shown effects on specific depressive symptom clusters including cognitive symptoms and anhedonia
- Research at Massachusetts General Hospital (Dr. Paolo Cassano's group) has produced some of the most rigorous tPBM-for-depression work to date, with positive findings in phase II trials
Honest Assessment of the Evidence
The findings are encouraging, and the mechanistic basis is sound. The limitations:
- Most positive trials are small (20-60 participants)
- Larger phase III RCTs are underway but not yet completed for psychiatric indications
- Heterogeneity in depression subtypes makes generalizable conclusions difficult
- Consumer-level NIR devices operate at lower irradiance than research devices
- NIR therapy for depression is not FDA cleared, approved, or an established treatment
The research trajectory is positive. The evidence is not yet at the level of established psychiatric interventions.
Practical Considerations for Home Use
Device Placement
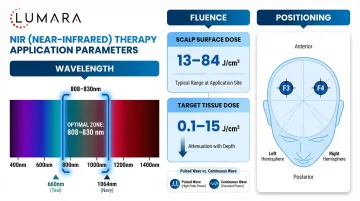
Transcranial NIR applications typically target the forehead (prefrontal cortex region) - the forehead area centered above the eyebrows and extending toward the temples. Some protocols also target the crown or posterior head.
Session Protocol from Research
Research protocols vary, but common parameters include:
- 810-850nm wavelengths
- 10-20 minutes per session
- 3-5 sessions per week
- 8-12 weeks for assessment of response
Consumer-level devices operate at lower irradiance than research devices, meaning longer sessions may be needed to approach comparable tissue doses. For best delivery, apply directly to bare skin with hair parted at the treatment site.

Important Safety and Clinical Context
- Do not modify psychiatric medications or treatment plans based on NIR therapy results without physician guidance
- NIR therapy is not a replacement for established depression treatments (medication, psychotherapy, TMS, ECT)
- Anyone with active suicidal ideation, severe depression, or complex psychiatric conditions should be managed by a mental health professional - not self-treating with light therapy
- Some research is examining tPBM for brain inflammation, post-traumatic brain injury, PTSD, and other neurological conditions - the evidence base varies by condition
How Lumara's Devices Relate to This Application
Lumara's primary device lineup targets skin wellness and body recovery - not transcranial neurological applications. However, Lumara's Illuminate V2 (660nm, 1,800 LEDs, 5 minutes, FDA cleared) is built around verified wavelength precision at irradiance levels relevant to surface and near-surface tissue applications.
For users exploring NIR for general wellness, stress resilience, and recovery applications (where NIR's mitochondrial support mechanism applies to muscle, joint, and general cellular health), Lumara's Illuminate V2 provides a high-quality 660nm platform. The device supports pulsed red light therapy delivery and eyes-open or eyes-closed session protocols depending on the application. For the transcranial NIR application specifically, the relevant research wavelength is 810-850nm rather than 660nm - meaning near-infrared-specific devices are more directly aligned with the research protocols for this application.
Frequently Asked Questions
Does near-infrared light therapy help with depression?
Small clinical trials have shown improvements in depression symptoms with transcranial NIR therapy. The evidence is promising but not yet definitive - large-scale RCTs are ongoing. It is not an established treatment and should not replace medical care.
What wavelength is used for depression in near-infrared therapy?
Most research uses 810nm or 850nm NIR wavelengths applied transcranially. These wavelengths penetrate through the skull to cortical tissue.
How long does it take for near-infrared therapy to affect mood?
Research protocols typically run 8-12 weeks. Some studies show early improvements in 2-4 weeks. Individual variation is significant.
Is near-infrared therapy safe for mental health conditions?
Consumer-level NIR therapy applied externally to the head is generally considered safe for most users. Anyone with active severe depression, suicidal ideation, or bipolar disorder should be managed by a mental health professional and should discuss any complementary approaches with their treating physician.
Can NIR therapy replace antidepressants?
No. NIR therapy is a complementary approach being studied for depression support. It is not approved or validated as a replacement for antidepressants, psychotherapy, or other established treatments.
Promising Science, Appropriate Context
Near-infrared light therapy for depression has a coherent mechanism and encouraging early evidence. It is not ready to be positioned as a treatment, but it is worth following as the clinical evidence matures.
For users building a general wellness and recovery routine that includes NIR light therapy, Lumara's Illuminate V2 provides precision wavelength delivery and consistent output for daily use.


