
Introduction
Pulsed red light therapy is marketed by some manufacturers as a premium feature - the claim being that pulsing the light output produces better results than continuous output. The reality is more nuanced, and for most at-home red light therapy applications, the pulsed vs continuous distinction matters less than wavelength accuracy and irradiance.
This guide covers what pulsed and continuous output actually are, what the research shows, and what should actually drive your purchasing decision.
Key Takeaways
- Continuous output delivers a constant stream of light during the session; pulsed output alternates between on/off cycles at specific frequencies
- Research on pulsed versus continuous PBMT exists but results are mixed - no consensus supports pulsing as universally superior for consumer applications
- Certain pulsed frequencies (particularly 40Hz near-infrared) have specific neurological research basis; this does not generalize to all pulsed devices
- Wavelength accuracy, irradiance at treatment distance, and coverage consistency are more impactful purchasing factors than continuous vs pulsed output
- Lumara's Illuminate V2 uses continuous 660nm output - optimized for consistent dose delivery and verified therapeutic wavelength
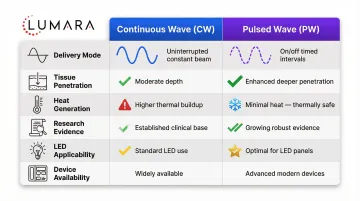
What Pulsed vs Continuous Actually Means
Continuous output: The LEDs emit a constant intensity of light throughout the session. The total dose delivered equals irradiance x time.
Pulsed output: The LEDs cycle on and off at a specific frequency, expressed in Hz (cycles per second). A 10Hz device cycles on and off 10 times per second.
The purpose of pulsing in research contexts is to explore whether specific frequencies produce different cellular responses than continuous light. In some clinical PBMT applications, pulsed frequencies are used to target specific tissue responses.
What the Research Shows
The 40Hz NIR Pulsing Research
The most substantive evidence for pulsed light in therapeutic contexts involves 40Hz near-infrared - specifically in neurological applications for conditions including Alzheimer's disease research. At 40Hz, near-infrared light exposure has shown effects on gamma oscillations in neural tissue in preclinical and early clinical research.
This is specific to 40Hz frequency and near-infrared wavelengths (850nm range) in neurological contexts. It does not generalize to: red light (660nm), skin applications, muscle recovery, or any other consumer use case.
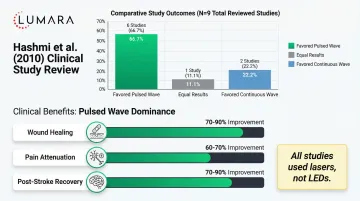
General PBMT Pulsing Research
Outside of the 40Hz NIR context, the research on pulsed versus continuous PBMT does not strongly favor either approach for common consumer applications. Some studies show benefits for specific pulse frequencies in specific applications; others show continuous output performing equivalently.
The honest summary: there is no strong, generalizable evidence that pulsed output is superior to continuous output for skin wellness, muscle recovery, or standard body recovery applications.
The Dose Calculation Issue with Pulsed Devices
This is a practical consideration many buyers miss.
When a device pulses at 50% duty cycle (on half the time, off half the time), it delivers half the dose of a continuous device at the same stated irradiance over the same time. This means:
- A pulsed device may need to run twice as long as a continuous device to deliver the same dose
- Irradiance measurements at the LED level for pulsed devices may reflect peak irradiance, not average irradiance - which is what determines actual dose delivered to tissue
Some manufacturers state irradiance for pulsed devices at peak output (when LEDs are on) rather than average output (accounting for the duty cycle). This can make pulsed devices appear more powerful than they are in practice.
Ask any pulsed device manufacturer: is the stated irradiance average (accounting for duty cycle) or peak (LED-on only)?
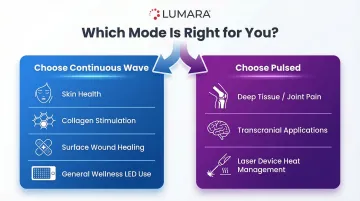
What Actually Matters More Than Pulsed vs Continuous
For most at-home red light therapy applications, these factors have more impact on results than pulsed vs continuous:
1. Wavelength accuracy: 660nm at the LED must actually be 660nm. Without third-party verification, stated wavelength and actual output may differ by 10-20nm - which affects whether the device hits the therapeutic window.
2. Average irradiance at treatment distance: The energy delivered to tissue over the session duration. For continuous devices, this is straightforward. For pulsed devices, confirm average irradiance accounts for duty cycle.
3. Coverage consistency: Even LED spacing ensures consistent dose across the treatment area. When comparing panel vs mask form factors, coverage and irradiance uniformity are key differentiators.
4. Session time and dose: More important to accumulate the right total dose than whether delivery is pulsed or continuous. The mitochondrial response to photobiomodulation depends on cumulative energy delivery, not delivery mode.
Lumara's Approach: Continuous Verified Output
Lumara's Illuminate V2 uses continuous 660nm output - not because pulsing is inferior in all contexts, but because:
- Continuous output makes dose calculation transparent and straightforward
- Stated irradiance is average irradiance - no duty cycle adjustment needed
- Triple-verified 660nm wavelength means the therapeutic window is confirmed, not assumed
- 5-minute session guidance is calibrated to deliver 6,000 joules at the verified irradiance
For users interested in 40Hz NIR pulsing for neurological applications, that is a specific context requiring near-infrared wavelengths (850nm range) - not the 660nm skin and body wellness application that Illuminate V2 is built for.
Frequently Asked Questions
Is pulsed red light therapy better than continuous?
Not generally. For most consumer applications - skin wellness, muscle recovery, body recovery - there is no strong evidence that pulsed output is superior to continuous. The 40Hz near-infrared pulsing research is specific to neurological contexts and does not generalize.
What is duty cycle in pulsed light therapy?
Duty cycle is the percentage of time the LEDs are on during a pulsed session. A 50% duty cycle means LEDs are on half the time. This affects total dose - a device with 50% duty cycle delivers half the dose of a continuous device at the same stated peak irradiance.
Does pulsing affect irradiance measurements?
Yes, and this is often misunderstood. Some manufacturers state peak irradiance (LEDs on only) for pulsed devices, not average irradiance. For dose calculations, average irradiance matters. Always confirm which figure is being stated.
What frequency should I use for red light therapy?
For skin wellness and body recovery applications, frequency of pulsing is not a primary variable. Focus on wavelength accuracy (660nm for skin, 850nm for deep tissue), average irradiance at treatment distance, and session duration.
Focus on What Determines Dose
Pulsed vs continuous is a secondary consideration for most at-home light therapy applications. Wavelength accuracy, average irradiance at treatment distance, and consistent coverage are the specs that determine whether a device delivers therapeutic dose.
Lumara's Illuminate V2 - 660nm triple-verified, continuous output, 1,800 LEDs, 6,000 joules in 5 minutes, FDA cleared - is designed around transparent dose delivery without pulsing ambiguity.


